|
Swing a light back and forth in front of the two pupils and compare the reaction to stimulation in both eyes. The swinging flashlight test is helpful in separating these two etiologies as only patients with optic nerve damage will have a positive RAPD. However, it will constrict if light is shone in the other eye (consensual response). 
If an optic nerve lesion is present the affected pupil will not constrict to light when light is shone in the that pupil during the swinging flashlight test. It is important to be able to differentiate whether a patient is complaining of decreased vision from an ocular problem such as cataract or from a defect of the optic nerve. It is due to damage inoptic nerve or severe retinal disease. Relative Afferent Pupillary Defect (RAPD, Marcus Gunn Pupil)Īn RAPD is a defect in the direct response. They synapse at the superior cervical ganglion where third-order neurons travel through the carotid plexus and enter into the orbit through the first division of the trigeminal nerve. Post synaptic neurons travel down all the way through the brain stem and finally exit through the cervical sympathetic chain and the superior cervical ganglion. Sympathetic innervation begins at the cortex with the first synapse at the cilliospinal center (also known as Budge's center after German physiologist Julius Ludwig Budge). Dilation is controlled by the dilator pupillae, a group of muscles in the peripheral 2/3 of the iris. Sympathetic innervation leads to pupillary dilation. The fibers enter the orbit with CNIII nerve fibers and ultimately synapse at the cilliary ganglion. The pathway of pupillary constriction begins at the Edinger-Westphal nucleus near the occulomotor nerve nucleus. The fibers of the sphincter pupillae encompass the pupil. A circular muscle called the sphincter pupillae accomplishes this task. Parasympathetic innervation leads to pupillary constriction. As the inferior oblique and inferior rectus muscles share the capsulopalpebral fascia, overly aggressive manipulation of the muscles during exposure of the orbital floor fracture may consequently lead to injury to the ciliary ganglion or the inferior branch of the oculomotor nerve, resulting in mydriasis on rare occasions.The physiology behind a "normal" pupillary constriction is a balance between the sympathetic and parasympathetic nervous systems. Postsynaptic parasympathetic fibers travel in the short ciliary nerves and reach the sphincter pupillae, causing constriction ( Fig. Once in the orbit, the parasympathetic fibers are located in the inferior branch of the oculomotor nerve and synapse in the ciliary ganglion. The parasympathetic fibers originate in the Edinger-Westphal nucleus in the midbrain and follow the oculomotor nerve into the orbit. Pupillary function is controlled by a balance of sympathetic (dilator) and parasympathetic (constrictor) neural pathways. Keywords: Anisocoria / Mydriasis / Blow out fractureĭuring orbital fracture surgery, potential causes for unilateral mydriasis include local anesthetic infiltration into the eyelids, orbit, and paranasal sinuses, manipulation of the inferior branch of the oculomotor nerve, manipulation of the ciliary ganglion, direct injury to the optic nerve, and globe injury. Anisocoria-related situations must be addressed in a proficient manner through sufficient understanding of the mechanism controlling the pupillary response to various stimuli. Moreover, surgeons must be aware of the fact that excessive injection of lidocaine with epinephrine for hemostasis during orbital wall surgery can result in intraoperative anisocoria. Preoperative ophthalmic evaluation is simple and essential in ruling out any preexisting neurologic condition. In conclusion, neurological and ophthalmologic evaluation must be performed prior to blowout fracture surgery. By 3 hours after the operation, the mydriasis had resolved with normal light reflex. After approximately three hours of the surgery, the ipsilateral pupil was observed to be dilated, with sluggish response to light. In total, 40 mL of local anesthetic was used for the duration of the operation. To control this bleeding, a 1% lidocaine solution with 1:200,000 epinephrine was applied to the orbital wall with cotton pledgets. During the operation, persistent bleeding occurred. A 54-year-old woman was struck in the face and was admitted for a medial blowout fracture of the left eye. We report a case of transient anisocoria occurring during medial blowout fracture reconstruction and review the relevant literature. 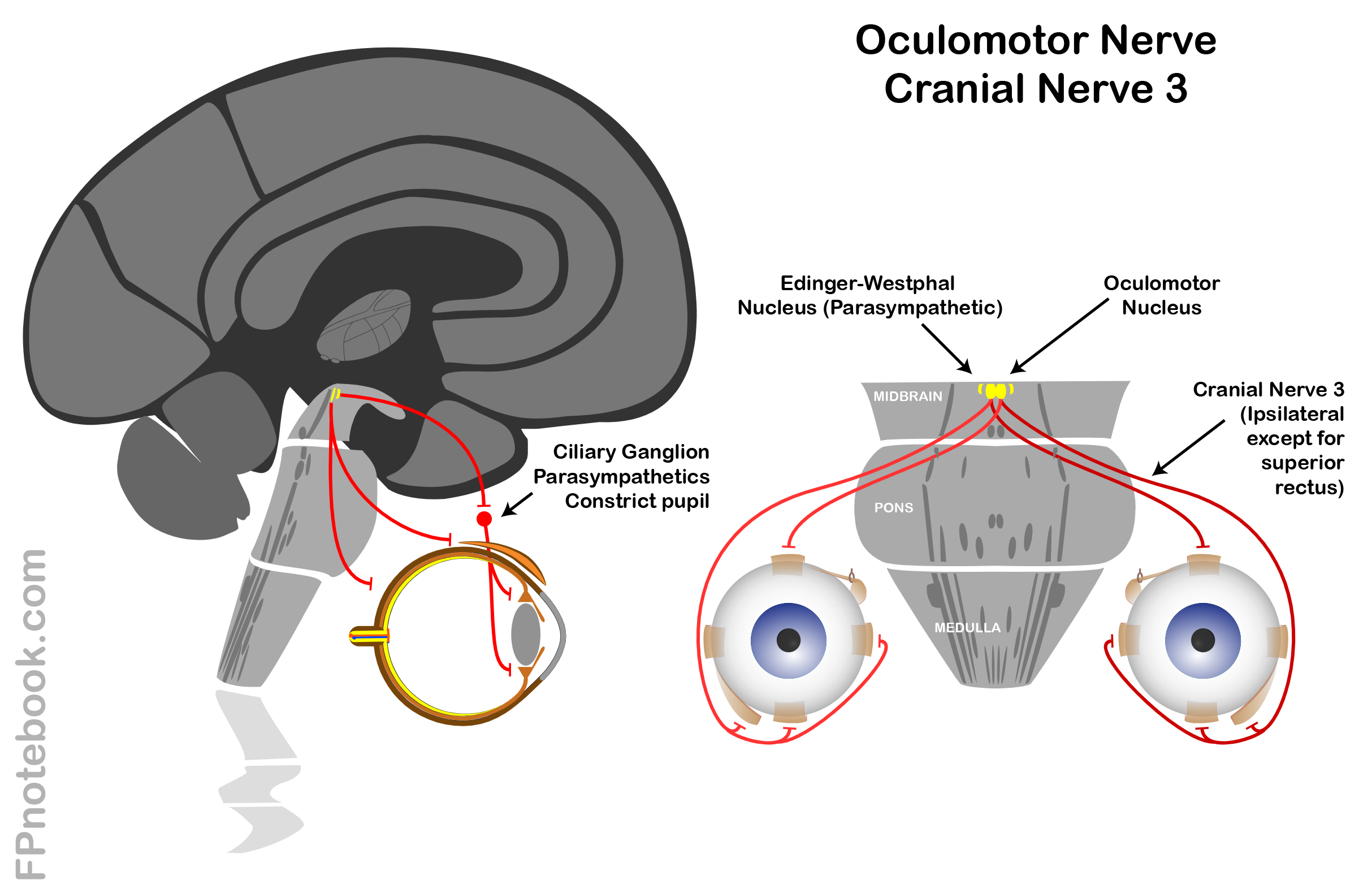
Transient anisocoria is rare during blowout fracture reconstruction.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
